The Mallory Foundation, a private foundation located in Carson City, announced a $200,000 donation to…
Another day in the Emergency Department: Roller Coaster of Emotions
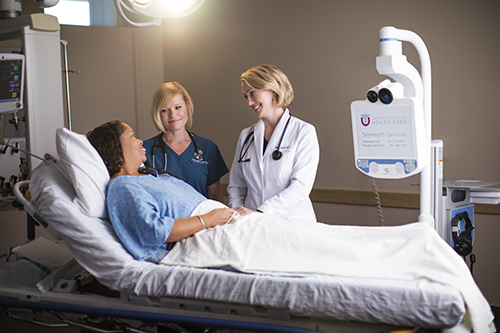
By Meg Jack, MD
Carson Tahoe Emergency Department Medical Director
The day-to-day life in the Emergency Department is similar to riding an unfamiliar roller coaster. It could travel at the leisurely speed of a rollercoaster for two-year-olds bought off Amazon or it be as gripping as Disneyland’s Space Mountain traveling in the dark with unpredictable speed and unforeseen twists, turns and ups and downs.
This particular day began just like any other but then hit alarming rollercoaster speeds with an explosion of critically ill patients. We were zipping around between rooms with an acute stroke, multiple septic patients, two intracranial hemorrhages, and a screaming elbow dislocation when a gentleman pulled on my heartstrings and brought tears to my eyes. He was a sweet man in his 60’s who thought he was just coming in with dehydration from his recent chemotherapy. Little did he know, he would be flying amongst the angels in less than 12 hours.
He had cancer. He thought it was under control until we realized it likely eroded through his intestines unleashing stool throughout his abdomen. His body was shutting down and going into shock and there wasn’t much we could do. Starting antibiotics would have been as helpful as holding a bucket when a flood is coming. We started him on medicine to help increase his blood pressure, not as a lifesaving measure, but to buy him time; time with his wife, children, best friends, and grandchildren. Time with the people one turns to during both wonderful and terrible times. I can give you time I told him; I’m just not sure how much time. So we proceeded to place special lines and start him on one, two and subsequently three medications to sustain his blood pressure to prevent him from rapidly dying. The most heart-wrenching part was this gentleman was actively dying and yet, he was sitting up in bed, conversing, and smiling. He wanted those last few conversations, another hug, and pictures and videos with his young grandchildren. Even as beads of sweat came over his face and his skin turned gray, there he was, making sure everyone around him was okay. His loving nature was so obvious and special. I asked if he was always so sweet and caring, and everyone said that he’s always been like that, and he was one of the best people they had met. When his surgeon arrived, she cried and felt helpless, as she couldn’t save him. We had every possible medical intervention at our fingertips, but trying to give him a few extra minutes or hours was all we could do. I had a lovely discussion with his loved ones about making this something that we call “a good death”. This entails filling the room with love, stories, hugs, and laughter with those most important. As his wife cried, I grabbed her hands and told her she can do this. And she did.
Before I left to go home, I checked on him again, and despite being so sick, we held hands and he said, “What’s up doc?” After our last words, his wife gave me a hug and he told me, “Have a safe journey home.” A man who was actively dying was concerned about my safety? WOW! I returned the next morning and was surprised he was still alive. He was gray and wouldn’t awaken. I grabbed his cold hand, told him he was a good man and then whispered in his ear, “Have a safe journey to heaven.” Subsequently, all of his medications were stopped, and he passed peacefully with his family and friends at his side.
When people arrive at the Emergency Department so sick that they are unable to speak to you, their departure is less emotional. But when you look into someone’s eyes, see their soul, hold their hand, and connect with them, letting them go is much harder. It’s the connection with people that brings out the emotion that we normally suppress to continue marching onto the next patient. It’s so heartbreaking to watch someone who is so wonderful leave this earth. It’s the paradox of the Emergency Department as we constantly try to understand why some of the most challenging patients who don’t care about themselves, their health, or those around them continue to live while some of the best die. I would like to think it’s because they are such good souls that they are needed in heaven.
Our jobs are hard: physically, mentally, emotionally, and spiritually. We see firsthand, the harsh realities of life. But we also see grace in those truths. As a healthcare provider, I can’t think of a better blessing than to be the one providing medical care, support, love, “a good death” in the end, and most gratefully, the beauty that arises from adversity.
*Patient gave consent to have this story shared.